Copy link
Carbon monoxide poisoning: Dx
Last updated: 03/04/2015
Carbon monoxide (CO) binds to hemoglobin about 200x tighter than oxygen. This results in
– Functional anemia (hemoglobin is unavailable for oxygen transport)
– Decreased oxygen delivery at tissues (left-ward shift of the oxygen-hemoglobin disassociation curve)
Provide immediate oxygen via a 100 per cent non-rebreather face mask, which will both promote cellular respiration and reduce the elimination T 1/2 of COHb from 4-5 hours to 1-2 hours. Always make a blood glucose determination and correct if necessary – extremes of glucose have the potential to exacerbate neuronal cell death. Continue oxygen therapy until the patient is asymptomatic (usually COHb < 10 per cent).
In case of persistent severe symptoms or markers of severe toxicity, consideration should be given to treatment with HBO. Many researchers advocate HBO for definitive treatment of severe symptomatic CO poisoning. The most obvious benefit of HBO is enhanced elimination of COHb, with a half-life average of 20 minutes at 3 atmospheres absolute. However, in reality most dissociation of COHb occurs with administration of normal pressure oxygen before HBO treatment. Therefore, the real benefit of HBO may be in regeneration of cytochrome oxidase and inhibition of leukocyte adherence to the microvascular endothelium. All this prevents the cascade of events that leads to ischemic reperfusion injury, the process thought to be responsible for lipid peroxidation of the brain and delayed neurologic sequelae.
Clear indications include 1) any loss of consciousness and 2) seizures, coma, or altered mental status. HBO should be considered 1) in patients with persistent neurologic symptoms, 2) in pregnancy, and 3) in patients with persistent cardiac ischemia. There are ways to optimize HBO treatment for CO poisoning. The first is that treatment should be performed as early as possible. In the only clinical series that retrospectively examined this factor, both mortality and delayed neurologic sequelae were substantially less in patients treated within 6 hours of discovery. Two recent controlled studies showed no benefit of HBO in poisoned patients when the average time to treatment was 6 hours. In contrast to these findings, a recent randomized trial showed a reduction in delayed sequelae from 33 per cent to zero, when patients were treated within 6 hours with HBO as opposed to routine oxygen.
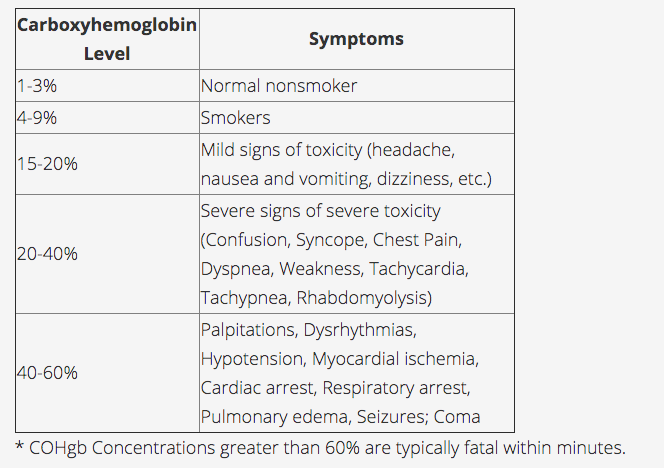
Carboxyhemoglobin Level-Symptoms Table
References
- I Blumenthal Carbon monoxide poisoning. J R Soc Med: 2001, 94(6);270-2 PubMed Link
Copyright Information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.