Copy link
Myotonic Dystrophy
Last updated: 05/30/2023
Key Points
- Myotonic dystrophy (MD) is characterized by muscle weakness and wasting (most prominent in the cranial and distal limb musculature), periodic myotonia, progressive myopathy, insulin resistance, and defects in cardiac conduction.
- The preoperative evaluation of these patients is crucial and should focus on cardiac, pulmonary, and gastrointestinal (GI) involvement and endocrine abnormalities, including diabetes and thyroid dysfunction.
- Anesthetic considerations include risk of aspiration, potential cardiac conduction abnormalities, avoidance of succinylcholine and neostigmine, and other methods to prevent myotonic reactions, including strict maintenance of normothermia and avoidance of shivering.
Introduction
- Myotonic dystrophy refers to a group of multi-system diseases characterized by myotonia, which refers to the abnormal and prolonged relaxation of a muscle following a voluntary (e.g., hand grip) or stimulated muscle contraction (e.g., electrical stimulation, hypothermia, shivering, percussion, administration of succinylcholine, etc.).1,2
- Two genetic forms of MD have been described: MD type 1 and type 2.
Myotonic Dystrophy Type 1 (Steinert’s disease)1,2
- Autosomal dominant inheritance
- Incidence: 1: 8000 (98% of all patients with MD).
- The principal defect is on chromosome 19.
- MD type 1 may present as congenital, childhood-onset, or adult-onset disease.
- It is characterized by muscle weakness and wasting (most prominent in the cranial and distal limb musculature), periodic myotonia, progressive myopathy, insulin resistance, defects in cardiac conduction, neuropsychiatric impairment, cataracts, testicular atrophy, and frontal balding in males.
- Importantly, the vocal cord apparatus is also involved.
- Mitral valve prolapse is present in 20% of patients.
Myotonic Dystrophy Type 2 (Proximal Myotonic Myopathy)1,2
- Quite rare (2% of all patients with MD)
- The principal defect is on chromosome 3.
- MD type 2 usually presents in adulthood and generally have less severe symptoms than MD type 1 patients.
- It is characterized by myotonia (90% of those affected), muscle dysfunction (82% weakness, pain, and stiffness), and less commonly, cardiac conduction defects, iridescent posterior subcapsular cataracts, insulin-insensitive type 2 diabetes mellitus, and testicular failure.
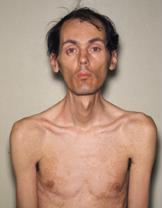
Figure 1. Typical appearance of a 40-year-old patient with MD with ptosis, muscle wasting, and frontal balding. Source: Wikipedia. Herbert L. Fred, MD, Hendrik A. van Dijk, CC BY 1.0. Link.
Preoperative Evaluation
A comprehensive preoperative should focus on the following organ systems:
- Cardiac: Both the myocardium and the His-Purkinje system can be affected, which can lead to cardiomyopathy and atrioventricular block/arrhythmia, respectively. Cardiac reserve and conduction abnormalities should be evaluated.
- Pulmonary: MD may affect a patient’s ventilation function and the ability to protect their airway. Pulmonary function testing usually shows restrictive lung disease.
- Gastrointestinal: Patients may have gastric atony and pharyngeal muscle weakness which predisposes them to gastric content aspiration.
- Endocrine abnormalities: Diabetes, thyroid/adrenal/gonadal dysfunctions
Anesthetic Considerations and Risks
Intraoperative management should aim to avoid triggering myotonia and should consider that MD patients are at an increased risk for the following:1,2
- Cardiac conduction abnormalities
- Aspiration secondary to delayed gastric emptying and weakness of pharyngeal muscles
- Hypersensitivity to the respiratory depressant effects of anesthetic agents and opioids
- Respiratory muscle weakness predisposes these patients to a weak cough and atelectasis.
- Metabolic abnormalities, including hyperkalemia and hyperglycemia
Monitoring1,2
- An arterial line allows quick identification of hemodynamic instability associated with cardiac conduction abnormalities and facilitates serial monitoring of serum electrolytes.
- Pacing equipment should be readily available for possible third-degree atrioventricular block refractory to atropine.
- Other invasive monitors may be considered, taking into consideration the patient’s preoperative cardiopulmonary status.
Induction1,2
- Etomidate, thiopental, and propofol have been used safely for induction. However, MD patients are more sensitive to these agents and a decreased dose should be used.2
- Weak pharyngeal musculature predisposes these patients to aspiration.
- Ideally, a rapid sequence induction without neuromuscular blockade should be performed.
- Avoid succinylcholine as it may induce exaggerated contractures, masseter spasm, laryngospasm, or severe hyperkalemia.
- If neuromuscular blockade is necessary, shorter-acting agents, such as rocuronium or cisatracurium, are favored.
Maintenance1,2
- Intravenous or inhalational agents are appropriate though there are limited case reports of myotonic reactions to etomidate and propofol.
- MD patients are no more susceptible to malignant hyperthermia than the general population.
- Deeper anesthesia is required for akinesia if neuromuscular blockade is not used.
Emergence1,2
- Neostigmine should be avoided for reversal of neuromuscular blockade as it may exacerbate myotonia.2
- Prolonged emergence can be expected due to hypersensitivity to anesthetic agents.
- Strict extubation criteria should be employed, given the patient’s increased risk for aspiration.
Environment
- Hypothermia and shivering can induce myotonia.
- Normothermia should be maintained with warm intravenous fluids and a forced warm air blanket, if necessary.
Regional Anesthesia
- Regional anesthesia has been successfully used as a primary anesthetic.
- Regional anesthesia can help reduce the risk of aspiration and sensitivity to anesthetic agents.
- Regional techniques may place the patient at increased risk of myotonia secondary to shivering and/or insufficient motor block to blunt the response to surgical stimulation.
Postoperative Care
- Close postoperative monitoring in an intensive care unit or step-down unit is warranted.
- MD patients are very sensitive to the respiratory depressant effects of opioids. Multimodal analgesia with regional anesthesia blocks, acetaminophen, and nonsteroidal anti-inflammatory drugs should be considered.
References
- Veyckemans F, Scholtes JL. Myotonic dystrophies type 1 and 2: anesthetic care. Paediatr Anaesth. 2013;23(9):794-803. PubMed
- Ferschl M, Moxley R, Day JW, et al. Practical suggestions for the anesthetic management of a myotonic dystrophy patient. Myotonic Dystrophy Foundation. www.myotonic.org. Accessed Mar 12th, 2023. Link
Copyright Information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.